By Jennifer Sicking
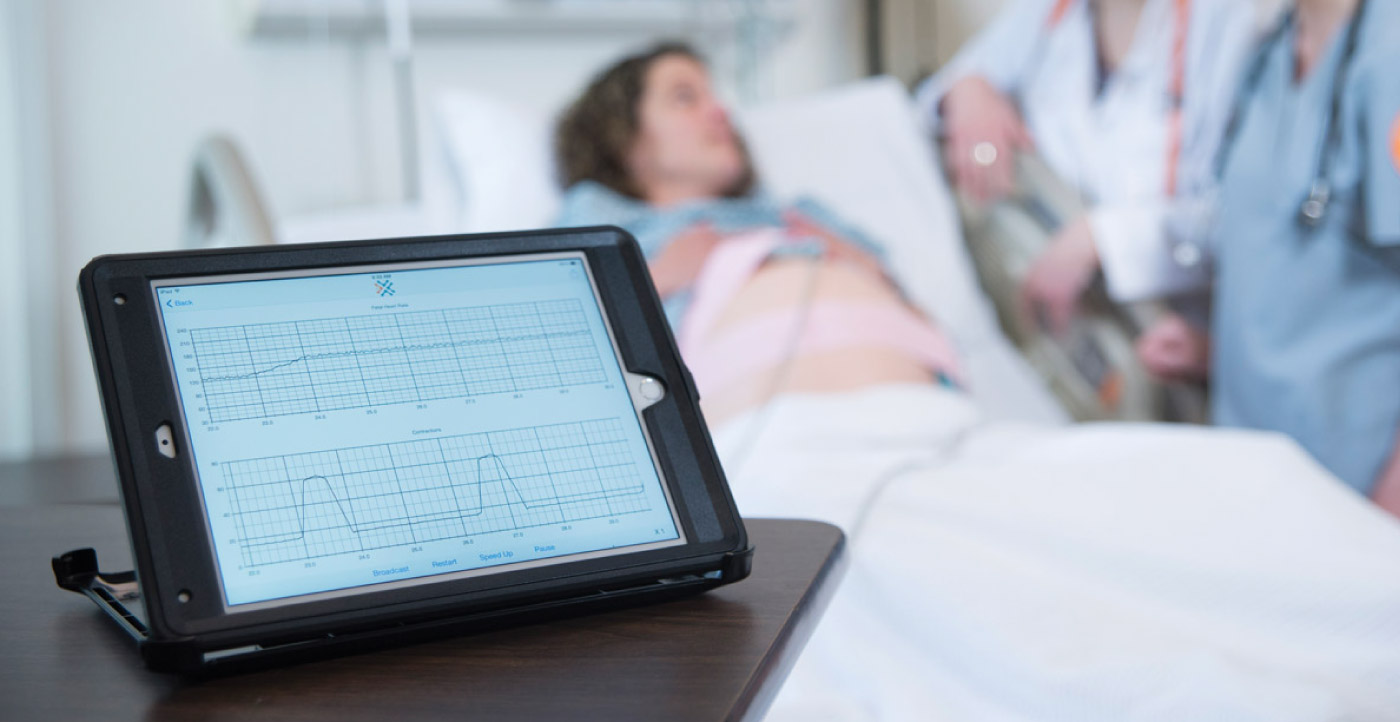
Sheila Taylor leaned in to see the baby’s heartbeat rhythm. She watched the line fall without a corresponding spike showing the mother’s uterus contracting. “That looks ugly,” she murmurs.
This time, there was no baby in distress. No hurried Caesarean delivery. It was all just a simulation—a University of Tennessee iPad app to train labor and delivery nurses.
University of Tennessee, Knoxville College of Nursing colleagues Taylor, a clinical assistant professor, and Susan Fancher, the simulation director, worked to develop the app to create a more realistic experience to instruct future nurses in monitoring babies and their mothers during labor. Xueping Li, associate professor of industrial and systems engineering, and Tami Wyatt, professor in College of Nursing, also helped develop the app.
“We love to collaborate with others,” Fancher says. “We have problems, and others can help us find solutions.” The app mirrors the latest evolution in fetal care.
Beginning in the 19th century, nurses and doctors used a fetoscope—a combination of a listening horn and a stethoscope—to hear a baby’s heartbeat. In the 1960s, doctors and nurses began using electronic fetal heart rate monitors to discover when a baby might run into a birthing difficulty. Fetal monitors printed out the birthing rhythms, showing the valleys and peaks of the baby’s heartbeat and the mother’s contractions, on continuous strips of five-inch-wide paper.
Now, U.S. hospitals have put more than 28,000 monitors to work, and banks of computer screens show continuous scrolls of the 10-second life increments between mother and infant. There’s a need for nurses to interpret the data. If nurses spot problems, such as the baby’s heart rate falling when the mother isn’t having a contraction, they call the health-care provider.
“The nurse is the expert in the room for fetal heart tracing,” Fancher says. For years, student nurses practiced reading signs in the paper strips. Now the app simulates the real world on iPads. Instructors set the baby’s heart rate, how often contractions happen and other options that, in real life, could spell trouble for the baby. Via the iPads, they broadcast the simulation to their students, who then practice interpreting the signs during the wonder of childbirth.

“We play with this for three hours,” Taylor says. “They know fetal monitoring when we’re through.”
Students also can download the app to practice interpreting the data on their own. While the UT nursing simulation lab is filled with lifelike mannequins for student practice, it has only one birthing mother mannequin. That mannequin’s price tag—$55,000—is a steep difference from the $5 mobile app for students and $25 for instructors.
After conducting trials with the app in summer 2014, the professors released it in 2015 and began using it in the classroom. Abbey Taylor and Alisa Melnikova, who graduated in May 2016 and began working at UT Medical Center in Knoxville as labor and delivery nurses, say the app matched their real-world experiences. “The whole point of simulation is to be the most realistic exposure that it can be,” says Melnikova.
When Abbey Taylor arrived at her field experience hospital, she watched the fetal heart monitors sending the patients’ updates, and her nerves quieted.
“It was like, ‘Oh, I’ve seen that,’” she says with a laugh. “It helped a lot to be prepared for that.”
Now, with the help of the UT Research Foundation (UTRF), more students around the world can use the app to learn. Since its release in 2015, the student version has been downloaded more than 100 times and the instructor more than a dozen. UTRF staff work with university faculty to license, patent and market their inventions.
“UTRF has been crucial to us to get it out there,” Fancher says.
Team members see great potential for the app as labor and delivery nurses must test for a certificate in fetal monitoring and document their competency in it each year.
“I think it will stay in the academic setting and migrate to the business setting,” Sheila Taylor says.